The explanation of benefits (EOB) is an important statement for every dental practice. It informs your billing team about the status of the insurance claim they’ve submitted to the payer. Whether it’s reimbursed, denied, or partially paid, all details are clearly mentioned in an EOB.
It’s important to read what’s written in a dental EOB. So, your team can update patient accounts with reimbursements or take further steps to collect the due amount on denials or underpayments.
But if you can’t understand the details and terms in an EOB, you might not be able to improve your practice’s financial health the way you should.
So, we’ll help you with that by guiding you through reading a dental EOB and implementing strategies for effective dental billing services and consistent cash flow.
What’s a Dental EOB?
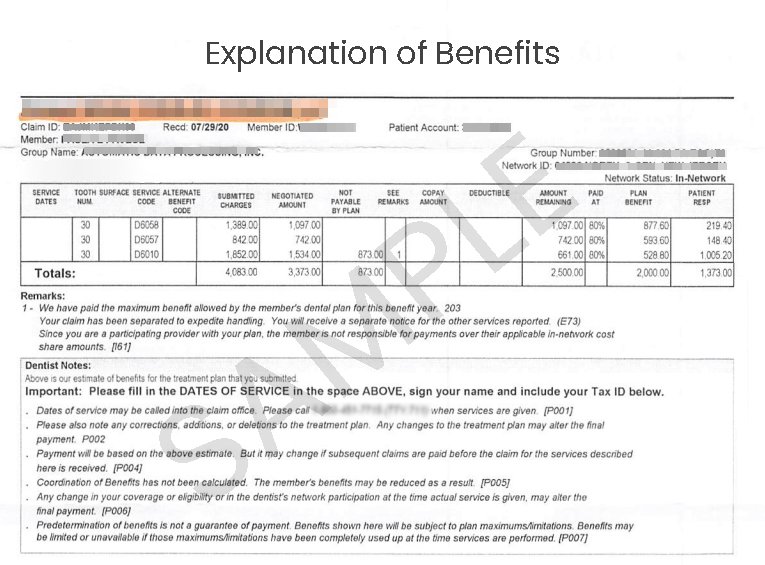
Before we discuss how to read a dental EOB, let’s understand what it is. The explanation of benefits is a document issued by the payer. In it, they state whether they’ve reimbursed a dental claim or denied it.
It includes all the details related to a claim, such as the:
- CDT code
- Service performed
- Billed charges
- Adjustments
- Actual reimbursements
- Remaining patient responsibilities
In short, the payer relates how they’ve received the claim, what they’re paying for it, and what the patient needs to pay.
What are the Components of a Dental EOB?
Now, let’s learn about the components in a dental EOB, so your team members, who handle your dental billing, know what’s in the statement and how to interpret it.
While each payer has designed their own dental EOB templates, key details are mostly the same. These include:
Patient and Provider Details
The dental EOB contains the details of the patient who has received the services and the provider who has performed the treatment.
Let’s see the details in the table below:
| Component | Description |
|---|---|
| Patient’s Name | The name of the patient who has received dental services. |
| Member ID | The identification number provided to the patient by the insurance company. |
| Group Number | An identification code of the patient’s group, which can be an employer plan. In this case, the employer’s insurance ID might be the group number. |
| Provider’s Name | The complete name of the dentist who has treated the patient. |
| Provider’s NPI Number | The National Provider Identifier (NPI) number is the dentist’s identification number registered in the NPI Registry. |
| Claim Number | An identification number that insurers use to track their records. Practices also use the ID to track claim status in the payer portal and EOB. |
| Payer Contact Details | The insurance company’s email address, office location, and contact number are provided, so the dental practice or patient can reach out to them for any queries. |
Date of Service and Procedure Code
A dental EOB mentions complete details related to a treatment, including the:
- Date of treatment/service
- Date of claim submission (Payer may write it as the date of receiving the claim)
- Date of claim processing
So, you can track if the date is correct, matching the date on which your provider has treated the patient.
It also contains the details of the dental procedure, including the CDT code, and a summary of the service, whether it’s a root canal, a cleaning, or any other treatment. This summary may appear as a Service Description in the explanation of benefits.
Financial Details
The EOB mentions all the details related to payment according to the payer’s contract with your practice. These include:
| Component | Description |
|---|---|
| Provider’s Charges / Billed Amount | The original fee of a provider, which they charge for dental procedures. It’s higher than the maximum amount insurance pays for the service. |
| Allowed Charges | The maximum costs of a dental procedure that the insurance company covers. |
| Covered Costs | The actual amount the payer reimburses for a dental procedure after adjusting for patient responsibilities like copays and deductibles. |
| Patient Responsibility | The treatment costs a patient pays after insurance covers its share. These include copays, deductibles, coinsurance, and non-covered services. |
Example: A patient visits your dental practice for a root canal on the front tooth. Your billed amount is $1000. Insurance reimburses a maximum of $800 for the treatment. By adjusting for a $50 copay and a $100 deductible, which the patient has to cover, the payer reimburses the remaining amount of $650. The table below shows how these costs are mentioned in the EOB.
| Provider Charges | Allowed Charges | Copay | Deductible | Covered Amount | Patient Responsibility |
|---|---|---|---|---|---|
| $1,000 | $800 | $50 | $100 | $650 | $150 |
Remark Code
Remark code is an alphanumeric code that explains why the payer denies a claim or makes adjustments before reimbursing the payment. Payers mostly use the standard Claim Adjustment Reason Codes (CARCs) or the Remittance Advice Remark Codes (RARCs).
These codes help you know the reason for a claim denial and underpayment, so you can correct the error and resubmit the claim. You can also avoid future errors in dental billing and coding by submitting clean and correct claims to ensure you’re paid on time and in full.
What are the Best Tips to Read a Dental EOB?
Here are a few expert tips for reading a dental EOB to compare details, correct mistakes (on your part), or request the payer to send a correct EOB.
Compare EOB Details with Claim Submission and Patient Records
Before you adjust a claim or post payment in the patient account, check if the details in the EOB match the exact procedure. Make sure that the CDT codes, service descriptions, and date of service are the same. Also, check and compare other details like:
- Patient name
- Member ID
- Dentist’s name
- Dentist’s NPI number
If details are missing or incorrect, immediately highlight the errors on the payer’s end and contact the payer. Attach a copy of the original claim with the patient’s treatment notes or charts, and prepare a description of the error in EOB. And submit the request to the payer to send the correct dental EOB.
It should be done within the payer’s deadline for claim escalation. It might be 30 days, 60 days, 90 days, or 180 days. Payer policy rules are different for every state and insurance company.
Also, document all your conversations with the payer representatives on EOB disputes, whether these are on the phone or via email. The payer provides you with a reference ID for the request, which you can use for follow-up.
Check Your Payer’s Remark Codes
Insurer’s remark codes in a dental EOB help you find the reasons for claim denials and underpayments. Don’t avoid these codes.
You can easily check the billing errors and work to fix them. Some common errors include:
- Wrong CDT code: The CDT code doesn’t match the actual treatment.
- Duplicate billing: The same claim has been submitted twice.
- Incorrect date of service: The date on the EOB is different from the actual date of treatment.
- Missed pre-authorization: The practice hasn’t received prior approval from the payer for treatments like crowns and bridges.
- Mistakes in patient and provider details: Patient’s name or member ID isn’t correct, or the dentist’s name or NPI doesn’t match the actual provider who has treated the patient. This may be due to spelling mistakes or missed numbers.
Payers can create their internal policy mapping, linking it to CARC and RARC, and deny claims or adjust payments according to that. So, consult their policies and provider manuals. They might also write a very brief description in the separate Remark Code section.
Example: A dentist submits a claim for a procedure using CDT code D2750, but the patient’s treatment record shows the procedure is D2950. Based on that, the payer mentions “CARC 16” in the Remark Code column in the EOB and writes a brief description of the denial: “Procedure code doesn’t match the treatment details.”
By using the denial code, you check your claim submission, and if the mistake is there, you make corrections and resubmit it with an appeal.
Document Your Dental EOB
Save all the EOBs with your claim details in the dental billing software, or if you’ve stored them manually, keep them in a single file with a copy of the original claim form and patient charts. It helps you match details with your claim to see if the payer has correctly processed it.
Comparison becomes quicker and easier, as you can check everything easily in one place. You don’t have to search in separate emails, portals, or patient files.
Plus, if you store these EOBs, you can use them in the future to identify repeated billing errors or constant claim denials on certain procedures. With that, your staff avoids these mistakes in future claim submissions. When claims are correct, EOBs are more likely to provide accurate results.
You can also prevent duplicate claim submission and payment posting with it, because payers mistakenly send EOBs twice for the same claim. If your staff doesn’t check the previous EOBs, they mistakenly post payments twice in the same patient account. So, by checking the previous EOBs, they can confirm what’s been paid. Accurate payment posting makes it easy to track revenue.
Automate EOB Checks
Your staff may take time to read EOBs, fix errors, or request the payer to submit the right EOB, which affects their productivity and slows down your cash flow.
You can make this process fast and smart with solutions like TransDental’s robotic process automation. The technology works on pre-set rules that automatically read the EOB, check the mistakes, and prepare appeal templates for claim resubmission. And all that happens in just seconds!
Automation reduces your time spent on manually checking EOB. While you still need to check for a final review, the results are almost accurate, so your final review doesn’t take much time.
What’s the Difference Between Dental EOB and Final Bill?
This is the point where billing staff and patients often get confused. They mistake the EOB for the final bill.
Due to that, the billing staff may charge patients incorrectly, and patients may end up paying the wrong amount. And when the patients complain to the insurers about that, it damages a practice’s relationship with the payer and the patient.
However, you can avoid that by clearing the confusion between dental EOB and the final bill.
Your staff must know the difference, so they bill actual charges to the patients.
The difference between the two documents is that the:
- EOB is just an information source on what insurance covers and what the patient pays
- The final bill is an invoice sent to the patient to notify them of their remaining charges after all the adjustments have been made.
Most insurance companies already explain in the dental EOB that it’s just information and not the final bill. As a result, there is no confusion.
Example: The payer covers $200 for a filling worth $250 in a patient’s coverage plan. After adjusting for the $20 copay and the $30 deductible, the insurer pays $150, and the patient must pay the remaining $50, as shown on the EOB. The practice generates a final invoice showing the total charge, insurance payment, and the $50 amount the patient owes.
Make sure that the patient charges on the EOB match the amount on the final bill. If you charge more, it can affect your relationship with the patient.
Conclusion
A dental explanation of benefits is an important document that tells you exactly what insurance covers and what they deny. Reading it shouldn’t be complicated. You must know what each section means, what denial codes stand for, and what to look for. You can catch errors or denials early, which saves your time. You can use that to fix errors and prevent them in the future, so claims are clean, payments are complete, and reimbursements are faster.
Frequently Asked Questions (FAQs)
What is an EOB for dental insurance?
An EOB shows how the insurer processed a claim, including payments, adjustments, and patient responsibility. It’s a summary of what was reimbursed or denied.
How long should a dental practice keep EOBs?
Keep EOBs at least as long as required by state law or payer rules, typically 6–7 years, to support audits, appeals, and accurate accounting.
What is the difference between EOB and a bill?
A bill is issued by the dental practice requesting payment, while an EOB is sent by the insurer showing what they paid, adjusted, or denied.
How do I read an EOB and find errors?
Compare the EOB to patient details and submitted claims, while checking CDT codes, dates, patient/provider info, and payment amounts. Flag discrepancies, reference CARC/RARC codes, and contact the payer for corrections.
Is an EOB a denial?
Dental EOB isn’t exactly a denial, but a statement that informs that a claim is denied and provides the reason for denial via a CARC or RARC denial code. Payer may also provide a summary of the denial reason in the EOB.